Feline Chronic Gingivitis Stomatitis (FCGS) syndrome
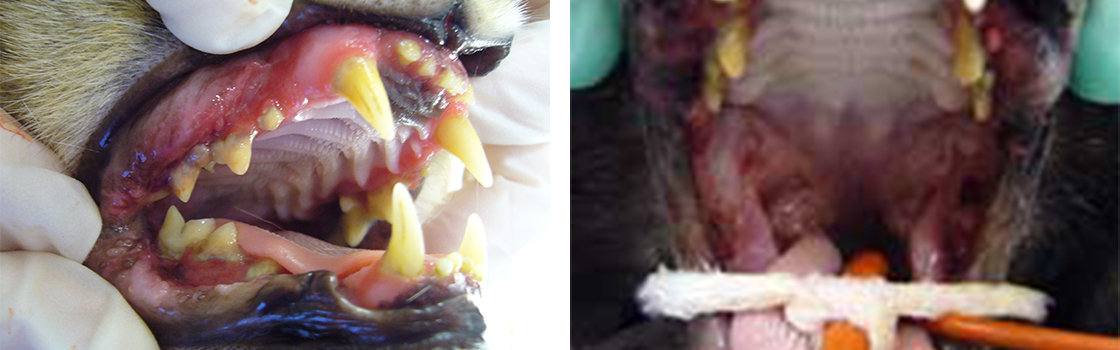
Case of FCGS - mild to severe presenting with caudal and alveolar mucositis.
FCGS cases make up a significant proportion of cat cases referred to us. FCGS has a reported prevalence of between 0.7% and 12% of cat dental cases seen in practice. Most cases improve dramatically with some form of medical or surgical treatment but a small proportion appears to resist all efforts. Much misinformation is available of the management of these cases, especially where novel treatments have been tried and where case numbers have been low without controls.
The driving factor for the extensive inflammatory changes appear to be an abnormal immune response to the oral antigenic burden - essentially dental plaque. Since plaque is a biofilm that cannot usually be seen without disclosure stains, this can make an oral assessment difficult. There are also several co-factors that interact together. However, plaque appears to be the main problem our primary efforts are directed at controlling this.
Our treatment and management protocol can be downloaded here. Be aware that a step by step approach to diagnosis and treatment are required and, as ever, step one is first!
It is essential that everything starts with a full assessment and chart of the mouth (including full mouth radiographs), dental scaling/polishing and identification and removal of teeth that have no future. Normally these will be teeth suffering from Feline Tooth Resorption (Feline TR) lesions or advanced periodontal disease. This is also an ideal time to take the various samples needed to asses general health and respiratory virus status.
If the lesions fail to improve with professional cleaning and chlorhexidine use twice daily it is likely that the antigenic burden is too high. Elective extraction of cheek teeth is now indicated. A recent review paper (Therapeutic Management of Feline Chronic Gingivostomatitis: A Systematic Review of the Literature; Winer JN, Arzi B, Verstraete FJM. Frontiers in Veterinary Science July 2016, vol 3, 54) indicated that elective near full-mouth extraction is the current standard of care for FCGS cases.
A combination of elective extractions of all premolars and molars, strict hygiene, oral chlorhexidine, antibiotics and feline interferon therapy is used in these refractive cases depending on response.
Immunomodulatory products, such as feline recombinant interferon omega, appear to be the next logical step in refractory cases in our opinion. Case selection is vital for interferon treatment as best results tend to come from cats that have already had elective cheek teeth extraction and are feline calici virus positive.
We have a large cohort of cases running since November 2007. Several other practices in the UK, Italy and France are working on similar lines. The success rates appear to show much promise in the management of such cases with either oral or injectable regimes.
One study by Hennet and others compared the use of interferon with other treatments.
Journal of Feline Medicine & Surgery (2011), 13, 577-587. Comparative efficacy of a recombinant feline interferon omega in refractory cases of calici virus positive cats with caudal stomatitis: a randomised, multi-centre, controlled, double blind study in 39 cats.
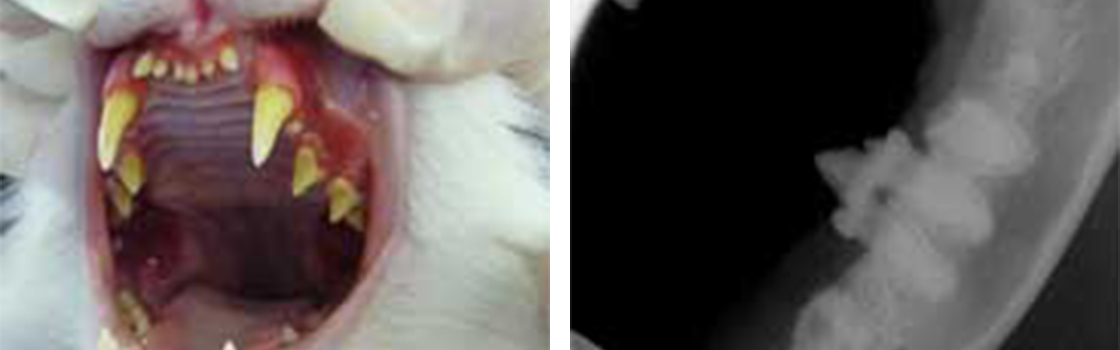
Typical case of FCGS Case radiograph showing retained roots.
From 2009 to 2012 we worked with both the University of Glasgow Dental and Veterinary Schools on a research project to determine the exact nature of antigen in the mouths of cats with this problem. The project used aerobic and anaerobic culture plus culture independent methods (gene sequencing) to find agents either hard to culture conventionally or novel species. Three papers have been generated so far from this study increasing our knowledge of the role of commensals in the mouth and also putative pathogens in these cases. Oral flora appears a lot less diverse in affected cats with Pasteurella multocida dominating in half the cases seen. The role of Tannerella forsythia as a putative pathogen has also been considered.
Many FCGS cats also test positive for Feline Calici Virus and this appears to be a co-factor within the complex inter-reactions that take place in these cases. We use the Scanelis lab in France to provide qualitative and quantitative PCR testing using their oral profile. Dry swabs in a vacutainer are fine they say - no cytobrush required. The virus burdens reported are a significant help in prognosis.
- Dolieslager SMJ, Riggio MP, Lennon A, Lappin DF, Johnston NW, Taylor D, Bennett D. Identification of bacteria associated with feline chronic gingivostomatitis using culture dependent and culture independent methods. Veterinary Microbiology. 2011 Feb 24; 148(1):93-8.
- Dolieslager SMJ, Bennett D, Johnston NW, Riggio MP. Novel bacterial phylotypes associated with the healthy feline oral cavity and feline chronic gingivostomatitis. Res Vet Sci. 2013 Jun; 94(3): 428-32.
- Dolieslager SM, Lappin DF, Bennett D, Graham L, Johnston N, Riggio MP. The influence of oral bacteria on tissue levels of Toll-like receptor and cytokine mRNAs in feline chronic gingivostomatitis and oral health. Vet Immunol Immunopathol. 2013 Feb 15; 151(3-4):263-74.
Check our updated download guidance notes:
Feline Tooth Resorption lesions (Feline TR)
Tooth Resorption (TR) lesions cause many problems in feline practice. Global surveys over the last 20 years indicate that 25% of the general feline population and 75% of those with other dental disease have at least one TR.
Extracting TR teeth is the only effective treatment and can be very difficult as the loss of normal landmarks and structure makes conventional root luxation often impossible.
In addition, TR lesions present as three distinct types (Type 1, Type 2 and Type 3). The types can only be identified and differentiated by dental radiographs. It must be noted that treatment for the three types is not interchangeable.
The appropriate extraction technique for type 1 lesions is conventional luxation via flaps and buccal bone plate removal. For type 2 lesions it can be coronectomy and alveoloplasty. These roots are already displaying bone replacement resorption. To attempt conventional luxation is to damage an area already healing. For type 3 lesions is can mean a mixture of the techniques for types 1 and 2 depending on radiographic appearance and gross presentation.
Good instruments are essential for feline tooth extraction. Our preference for feline dentistry is to use the "EX5" series luxators available from www.drshipp.com. Be aware of cheap imitations. Poor quality steel cannot be milled to produce blades this thin and sharp. Small teeth need nice instruments to remove successfully. To large a blade is prone to fracture the root.
Also, never be tempted by the "atomisation" option! Severe damage can and does occur to collateral structures without due care. The radiograph below illustrates what can happen with "root atomisation". The drill has passed though the ventral alveolar canal and presumably shredded its contents of blood vessels and sensory nerve to the whole mandible including soft tissue, bone and teeth. This technique has no place in veterinary dentistry.
Many cases of Feline Oral Facial Pain syndrome (FOPS - see below) arise initially from "tooth root atomisation" procedures. Most teeth have large sensory nerves (infra orbital or inferior alveolar) close to the apices of the roots. Atomisation procedures often go beyond the root apex damaging the nerves. Our advice? Don't do it!
For our most up to date information on Feline Tooth Resorption lesions please visit this link.
Feline Epulis
Feline Epulis is a rare condition that can be easily confused with cases of FCGS. This is a benign neoplasm of the periodontal tissues that support the teeth and surgery to remove the masses and associated teeth is generally curative. In some refractory cases radiation therapy may be helpful.
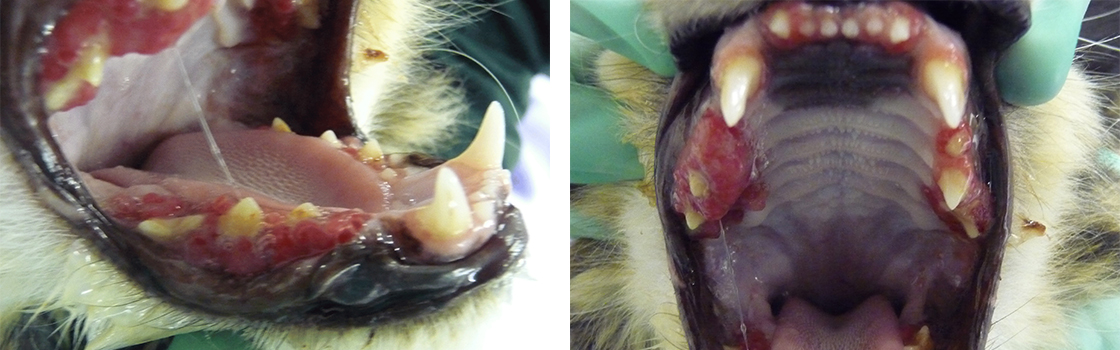
Feline Epulis case. Note friable hyperaemic gingiva all four quadrants. Case resolved with cheek teeth extraction all four quadrants.
Feline Oral Facial Pain Syndrome
A relatively uncommonly reported condition that mostly, but not exclusively, affects Burmese cats. Affected individuals demonstrate a complex of signs including frantic clawing of the face causing much self-inflicted damage. Many drugs have been used, including anti-anxiety drugs, to moderate or reduce the effects. The cause has not been established but it is likely to be multi-factorial. If you have a case please make contact by e-mail: a database will help in research.